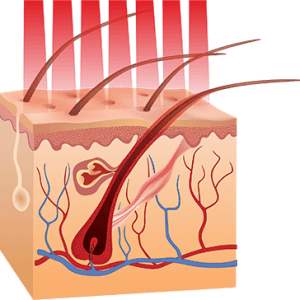
About Low-Level Laser Therapy for Hair Loss
Did you know? Low-Level Laser Therapy for hair loss is not a new or unproven treatment. In fact, it has been shown to be effective in numerous scientific studies, starting with its discovery almost 50 years ago.
In 1967, Hungarian scientist Endre Mester was working fervently in his laboratory. He was studying the healing effects of red laser on tumors in mice. The first working laser technology had been invented only several years prior. Mester was attempting to replicate an American colleague’s experiment, who had shown that a red laser could cure tumors implanted in a hamster.
Mester performed delicate surgery on each of his subjects, shaving the site for incision and implanting the tumor tissue. He then illuminated this surgical site with a red laser for carefully measured periods of time. Unbeknownst to Dr. Mester, however, his laser contained only a fraction of the power used by his American colleague. Needless to say, he did not cure any of the tumors. But he did notice something else: increased rates of wound healing and hair regrowth.

Dr. Endre Mester – A pioneer in the field of Low-Level Laser Therapy
These astute observations gave birth to the field of Low-Level Laser Therapy, or LLLT (also known as Low-Level Light Therapy, Photobiomodulation Therapy (PBM), or cold laser therapy). Subsequent experiments showed that low-intensity red laser had very unique biologic effect on cells, tissues, and organisms. Namely, LLLT was found to relieve pain, heal wounds, and regenerate tissues, restoring their natural form and function.
How does laser therapy fight hair loss and regenerate tissues? This is due to the fact that specialized molecules within our cells are able to convert the energy of red light into a usable form, in a similar way that plants can use energy from sunlight to grow and sustain themselves. More specifically, the enzyme cytochrome-c-oxidase within the mitochondria of our cells is energized by red light in a way that enhances cellular respiration, the process by which cells convert food, water, and oxygen into the energy we use to function and remain alive.
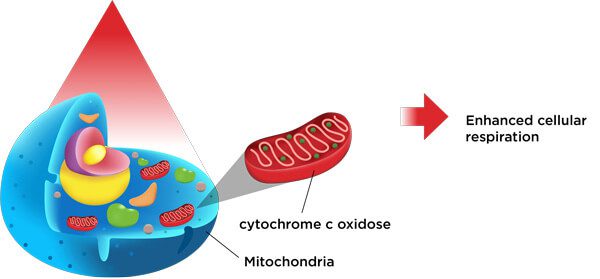
Cytochrome c oxidase, a specialized molecule within the mitochondria of our cells is energized when it absorbs red laser light. This enhances the process of cellular respiration, allowing cells to function more efficiently.
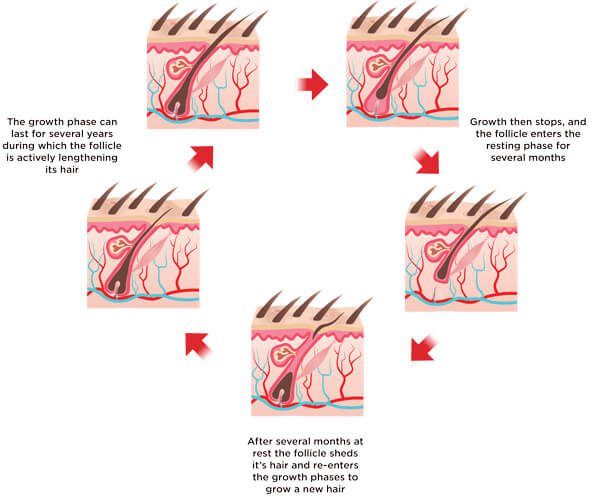
So what happens when laser therapy is used for hair loss? As discussed on our Hair Loss 101 page, each hair on your head grows in a characteristic cycle with several phases. The hair follicle will first spend several years in the growth phase, during which the hair actively lengthens. Next comes the resting phase, where the hair stops growing for several months. After a few months at rest, the follicle sheds its hair, the cycle begins anew, and the follicle begins to grow new hair.
When men and women are affected by androgenic alopecia, their hair follicles essentially shrink over time, and the growth phase becomes shorter and shorter with each cycle. As a result, each cycle produces a hair shorter and thinner than the last, a process called miniaturization.
The Hair Cycle
LLLT works by slowing, and in some cases, reversing miniaturization. When the scalp is illuminated by a red laser, light energy is absorbed by stem cells in the dermal papilla, a specialized region of the follicle near its base. These cells, which play a central role in controlling the hair cycle and promoting hair growth, are energized when they absorb red laser light, enhancing their ability to perform cellular respiration and and their metabolic efficiency.
As a result of this increased activity and a complex series of cellular and biochemical interactions, laser therapy for hair loss causes the hair follicle to spend a greater amount of time in the growth phase of the hair cycle, thereby slowing or reversing miniaturization and the progression of thinning and balding. Blood flow is increased as well via these interactions, delivering much-needed nourishment to sustain the follicle.
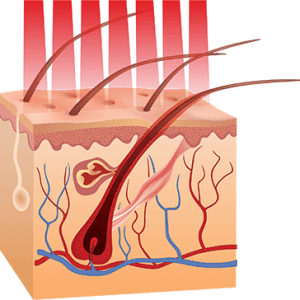
Red laser light energizes stem cells in the dermal papilla, deep within the hair follicle. As a result the length of the follicle’s growth phase is increased, and it produces a thicker, healthier hair.
Today, numerous high-quality clinical studies have shown LLLT to be an effective treatment for pattern hair loss.¹ In fact, LLLT is one of only three treatments sanctioned by the FDA for male pattern hair loss (along with minoxidil and finasteride), and one of only two treatments sanctioned by the FDA for female pattern hair loss (along with minoxidil). Laser therapy for hair loss has also been proven to have an excellent safety profile, and, unlike many other treatments for hair loss, is not associated with any serious adverse side effects.
Finally, LLLT can work for everyone, both men and women, and along with all other medical and surgical treatments for hair loss, including minoxidil, finasteride, platelet-rich plasma, hair transplant surgery, and more. For these reasons, we believe all people suffering from hair loss should use LLLT, with only the best – that is – The Original LaserCap!
- Liu K-H, Liu D, Chen Y-T, Chin S-Y. Comparative effectiveness of low-level laser therapy for adult androgenic alopecia: a system review and meta-analysis of randomized controlled trials. Lasers Med Sci. 2019;34(6):1063-1069.

Learn more about The Original LaserCap!
Restore Your Hair With LLLT